COVID-19 & Paxlovid: Day 0, Testing Positive & Getting Prescribed
Tagged:COVID
/
PharmaAndBiotech
Today your humble Weekend Editor finally tested positive for COVID-19. Sigh.
The Evidence
Last Saturday, I ventured forth from Château Weekend to have lunch with a friend visiting from out of town. I’ve only done that maybe twice in the last 2 1/2 years, so this is not exactly a frequently-taken risk.
And yes, I wore a mask even though it seemed nobody else did. “COVID’s over!”, they all seem to think. Yeah, right. Sure, kid. Whatever you say.
However, the north part of Boston’s MBTA Red Line was shut down completely for track/signal work, and so they shoved people onto crowded shuttle buses for an hour’s trip that would have been 15min by train. There, mask or no, I was in close quarters with many young people apparently so convinced of their invulnerability that they felt no need to mask.
All it would have taken was the slightest slip of my mask, or even just a virus laden droplet drifting into my eye.
Apparently, that’s what happened: Late Sunday afternoon, I started feeling achy and tired. By evening, I was running 1.5°C fever. This morning, it was 2.1°C and even more aches.
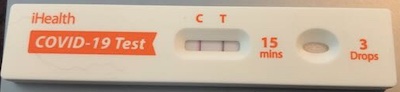 With a sense of dread, I took the test, whose results you can see here. Your humble
Weekend Editor definitely has COVID-19, at long last.
With a sense of dread, I took the test, whose results you can see here. Your humble
Weekend Editor definitely has COVID-19, at long last.
“Serves him right”, some of you are probably thinking, “for hectoring us about vaccinations and masking for 2 1/2 years!”
Well, go ahead and think that if you like. It was still the right thing to do. I got infected (apparently) because a random rail accident forced me onto a crowded shuttle bus full of unmasked young folk, whereupon even the slightest slip on my part was enough for Omicron/BA.5 (presumably) to take up residence.
The American healthcare double-bind
Now, to deal with the inherent cruelties of the American healthcare system. The doctors and nurses all seem quite compassionate and motivated, but the insurance, hospital, and practice bureaucracies are cruel.
See, we had to switch physicians. Our old one retired, so good for her. The new one, recommended by a friend in our religious community, couldn’t schedule us for new patient visits for 4 months. During that interval, our prescriptions would of course run out. The new doctor couldn’t prescribe, because she hasn’t seen us; the old doctor can’t prescribe because she is retired.
Eventually we got a nurse practitioner in the old doctor’s practice to write a “bridge prescription” until we could get in to see the new doctor. My new patient visit was to be this Wednesday.
But now, with COVID-19, the new doctor can’t see me. She can’t write prescription renewals and can’t prescribe paxlovid, because she hasn’t seen me. The old doctor is long gone, and the staff of that practice is now dispersed.
So… what to do?!
Sense and sensibility
Sometimes I’m fond of telling people, “Are you gonna break the rules, or are the rules gonna break you?”
So I was pleased when the new doctor’s staff, with eminent sensibility at a pleasantly surprising level, suggested:
- A telehealth visit today with a nurse practitioner to evaluate me for paxlovid, and
- A telehealth visit later with the doctor herself to establish care and allow her to renew existing prescriptions, so the new patient visit can be delayed (probably for months, alas).
We’ll see how that goes.
Paxlovid interview
I like nurse practitioners. Every encounter I’ve had with one has been sensible, calm, and straightforwardly guided to a solution. A good doctor is great, but doctors in general seem to be more of a mixed bag. But if you have a somewhat straightforward problem with a somewhat straightforward solution, and just need someone to do it… NP’s are your best friends.
And so it was here. She (and it’s almost always a woman, for no obvious reason) was very friendly, clear, and drove straight to the point. She figured out that I already knew a fair bit about paxlovid, so we could get through the medication interaction warnings and so on pretty quickly. She sent a prescription to my neighborhood pharmacy, and said it would be there “momentarily”.
The Weekend Editrix said she’d pick it up after her lunch.
I also got notification that my doctor’s appointment could be made virtual, to formally establish care, so she could then renew prescriptions.
So far – pending actually getting my claws into a box of paxlovid – this is looking like a success story all around. The new doctor appears to have a very practical, functional practice, and the nurse practitioner was as awesome as I’d hoped.
Veni, veni paxlovid!
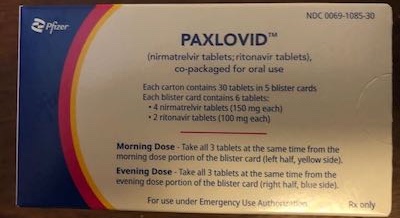
 All right, then: after a quick sail in the Weekend Zeppelin, the Weekend Editrix brought
home a box of paxlovid, shown
here. (Zero charge, even, with our insurance.) I looked at this with approximately the
level of anticipation of a 5-year old seeing a box containing a holiday present! (Now,
now: don’t judge me.)
All right, then: after a quick sail in the Weekend Zeppelin, the Weekend Editrix brought
home a box of paxlovid, shown
here. (Zero charge, even, with our insurance.) I looked at this with approximately the
level of anticipation of a 5-year old seeing a box containing a holiday present! (Now,
now: don’t judge me.)
It comes with the usual package insert full of a huge amount of tiny, tiny type explaining various things in technical gobbledygook and warning of dire consequences if… something-something. This is, of course, read by absolutely no one, being there mostly as a legal behind-covering move. (I’m only showing 1 of 2 big pages here, but it doesn’t matter since neither of us is going to read it, right?)
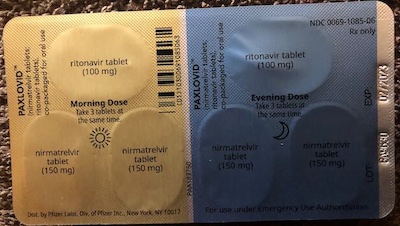
Inside there are 5 blister packs, divided into morning and evening doses. Each dose is 2 nirmatrelvir (the inhibitor of the viral “main protease” required for viral reproduction) and 1 ritonavir (which inhibits CYP3A4/P450-3A4, the liver enzyme which would ordinarily break down nirmatrelvir).
Ok, it’s now 3pm on the first day of testing positive. That’s close enough to “evening” for me. First dose down!
- The ritonavir tab is nondescript white. The nirmatrelvir tab, amusingly enough, is pink with “3CL” embossed on it. The other name for the main protease (“Mpro”) target, is the 3C-like protease (“3CL-pro”). Not many drugs are embossed with the name of the molecule they target! (On the other side of the pill, they embossed “PFE”, the stock ticker symbol for Pfizer. Sigh.)
- The taste is… nothing I particularly want to remember. I’m going to be having a metallic taste in my mouth for the next 5 days… and I’ll be grateful for that!
The Weekend Conclusion
Getting COVID-19 is a failure, probably because I was insufficiently pessimistic about getting on a crowded shuttle bus on Saturday.
But getting COVID-19 treatment fast, has thus far been a success.
Notes & References
1: Nope.

Gestae Commentaria
What are your estimates for your own personal odds of hospitalization and/or death conditional on:
First, welcome to the Weekend Commentariat!
Second, I like you: you’re asking the questions I probably should have asked, but I just went with my gut instead. Someday, I’m gonna learn to do better.
Still, the data is there: on 2022-Jun-02, I blogged about a very nice Israeli study on paxlovid in the wild, i.e., what response they observed on actual patient populations instead of in clinical trials. This is as real as it gets.
Some facts, for people aged 65+ like me:
Indeed, I suspect a vague recollection of those 2 facts and some knowledge of the safety profile of paxlovid (very safe) led me to jump at the chance to get it. But honestly, I was feeling pretty sick and a little scared, so I did what seemed like the safe thing.
Now specifically to your probability questions: I pulled the numbers out of the Israeli paper (see the table in the blog post above’s section called “The topline result”). For people age 65+, it looks like the numbers are (with error bars I haven’t bothered to figure out, but could):
Those imply a reduction in hospitalization of $100\% \times (1.9 - 0.6) / 1.9 = 68\%$, and a reduction in death of $100\% \times (0.4 - 0.1) / 0.4 = 75\%$. That doesn’t quite match their quoted reductions of 67% and 81% above, but it’s close.
The difference we can ascribe to the fact that, having access to the whole dataset, they could do a Cox proportional hazards analysis that takes into account dropouts from the trial. That’s the thing to do when you have real data, not just a crude overall average like I’ve done here.
So, there you go. I believe I’ve reduced my risk of hospitalization and death by a considerable factor. You might, perhaps, take the alternative view that those risks were low already and not worth bothering about. When it’s my own personal body at risk, I chose to take relatively easy, safe, and straightforward steps to reduce that already small risk. I have umbrella insurance for the same reason.
I hope that answers your question?