Paxlovid in the Wild
Tagged:COVID
/
JournalClub
/
Math
/
PharmaAndBiotech
An Israeli group has studied the use of paxlovid to treat COVID in a large group of age-stratified patients vs the SARS-CoV2 Omicron variant. The results are interesting, and a bit different from what I’d expected.
Paxlovid in actual practice
We’ve spilled a lot of ink on this crummy little blog that nobody reads about the discovery and clinical trial results of paxlovid. But as with many things in life, lab and trial results sometimes do not reflect the results you’d get in actual combat use. For example, paxlovid was tested only on:
- unvaccinated people; does it work as well on the vaccinated?
- older viral variants; does it work as well on Omicron?
So it’s always interesting to know if actual patients see the benefits we thought.
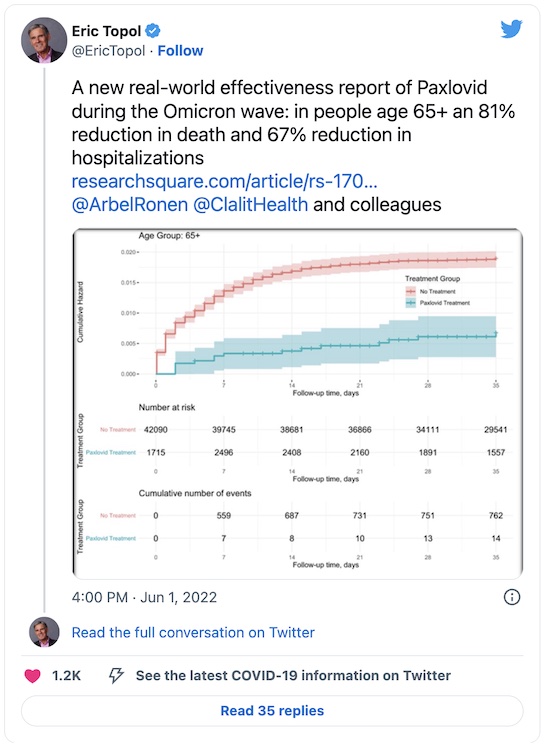
A study doing exactly that was first brought to our attention by the indispensable Eric Topol:
 It’s from an Israeli group associated with Clalit Health Services and Ben-Gurion
University who did the study [1], now available as a
pre-print pending peer review. Israel has actual universal health care with compatible
EMR systems, so they can do research that here in the benighted US we simply cannot do.
It’s from an Israeli group associated with Clalit Health Services and Ben-Gurion
University who did the study [1], now available as a
pre-print pending peer review. Israel has actual universal health care with compatible
EMR systems, so they can do research that here in the benighted US we simply cannot do.
Let’s see what it says!
The topline result
First, while paxlovid was developed during the Delta variant, they wanted to test the most relevant threat, namely the current Omicron variant:
Therefore, our objective was to assess the effectiveness of nirmatrelvir therapy for preventing mortality and hospitalizations due to Covid-19 in high-risk patients during the omicron surge.
Good for them. Much more relevant data in that case. (You can also tell this from the use of “omicron” in their title.)
 Their abstract mentions 109,213 participants, which they stratified into 2 eligible
populations: 42,819 age 65 or above, and 66,394 patients ages 40-64. Then some in
each group got paxlovid, while the rest did not.
Their abstract mentions 109,213 participants, which they stratified into 2 eligible
populations: 42,819 age 65 or above, and 66,394 patients ages 40-64. Then some in
each group got paxlovid, while the rest did not.
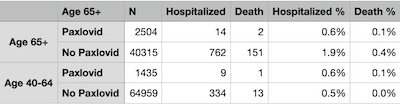
I took the numbers from their abstract and formatted them in the table shown here.
- The group sizes all add up properly to the total number of patients, so no issue there. (Though I did have to infer the number in each group not getting paxlovid by subtraction. Given censoring effects, this isn’t quite right, but the more subtle Cox proportional hazards analysis they did is in fact the right thing.)
- Pretty clearly there’s a dramatic benefit for those over 65: 3x less hospitalization % and 4x less death %.
- Also pretty clearly, there’s no such benefit for the 40-64 crowd: hospitalizations and deaths were within 0.1% of each other, well within the noise limits for a study like this.
 We could do our usual Fisher Exact Test here, to prove that quantitatively. However,
Arbel, et al. did a more sophisticated analysis using Cox regression to handle censoring
issues, which is the much More Correct Thing to Do (and which we cannot duplicate with
just the data in the paper).
We could do our usual Fisher Exact Test here, to prove that quantitatively. However,
Arbel, et al. did a more sophisticated analysis using Cox regression to handle censoring
issues, which is the much More Correct Thing to Do (and which we cannot duplicate with
just the data in the paper).
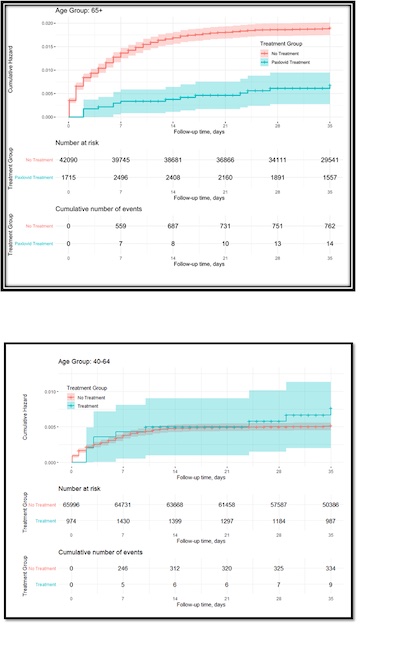
Have a look at the Kaplan-Meier curves, taken here from their Figure 2:
- The figure doesn’t say so, but matching number of events to the table we see this is for hospitalization rates in each arm. They apparently didn’t do a similar set of KM curves for the death rate, though it probably would have looked similar to this.
- The top plot is for ages 65+:
- Clearly the blue curve (paxlovid) and its 95% confidence interval stay well below the red curve (no paxlovid) and its 95% confidence interval.
- They quote a Hazard Ratio of 0.33 (95% CL: 0.19 – 0.55) for hospitalization and 0.19 (95% CL: 0.05 – 0.76) for death. Being bounded well below 1, these are highly statistically significant and have a meaningful effect size.
- The bottom plot is for ages 40-64:
- Note that the blue and red curve do not meaningfully separate; not only are they not outside each other’s 95% confidence limit, they’re practically on top of each other.
- They quote a Hazard Ratio of 0.78 (95% CL: 0.40 – 1.53) for hospitalization and 1.64 (95% CL: 0.40 – 12.95). Being not bounded below 1, these are not statistically significant (which you can just see from the plot, too).
The Weekend Conclusion
This is pretty nifty: it’s relevant to the current Omicron strain, and it’s on a heavily vaccinated population (Pfizer, mostly, in Israel). It’s high-quality data because they have a unified EMR system.
It says:
- For ages 65+: Paxlovid had a dramatic positive effect in reducing hospitalization and death rates.
- For ages 40-64: Paxlovid had not much effect at all on either hospitalization or death rates.
Though to be fair, the risk rates on younger people were much lower in the first place! Perhaps a fair summary would be that paxlovid made older people have the same risk rate as younger people?
Notes & References
1: R Arbel, et al., “Oral Nirmatrelvir and Severe Covid-19 Outcomes During the Omicron Surge”, Research Square preprint, 2022-Jun-01. DOI: 10.21203/rs.3.rs-1705061/v1. ↩

Gestae Commentaria
Comments for this post are closed pending repair of the comment system, but the Email/Twitter/Mastodon icons at page-top always work.