US pauses JnJ vaccine on thromboses
Tagged:COVID
/
MathInTheNews
/
PharmaAndBiotech
Today the US regulatory agencies “paused” the use of the JnJ COVID-19 vaccine to investigate thromboses, similar to what’s been seen with the AZ/OX vaccine. How many, how bad, and what will a pause do?
What’s the sitch in general?
We’ve been following closely the situation in Europe, where the AstraZeneca/Oxford vaccine has been scrutinzed for clotting disorders, specifically cerebreal sinus vein thromboses:
- Initially, it looked like nonsense because the rate of thromboses in the vaccinated population was lower than the background rate in the general population.
- Then it was restricted to a particularly rare cerebral sinus vein thrombosis (CSVT; aka cerebral venous sinus thrombosis, or CVST), but that looked like a statistical failure to do multiple hypothesis test correction.
- Then it was isolated into a specific population (younger women), and there were some mechanisms observed (PF4-heparin antibodies) and some unique characteristics (low platelet count/thrombocytopenia)… and I decided it was now so far outside any minor expertise of mine that I should back off & admit there might be something rare, but real happening here.
It still looked in the case of AZ/OX like the risks of not vaccinating the general population were far higher than the risks of thromboses, so vaccination should continue. But once there was a particular population identified (younger women) whose risk of dying from COVID was less than their risk of dying from thromboses, stopping was the right thing to do. So now the European authorities recommend AZ/OX for older patients with an age threshold depending on the country.
What happened to the JnJ vaccine today in the US?



 Today, though, the US authorities announced similar, but very rare, effects from the JnJ
vaccine. Both JnJ and AZ/OX are viral vector vaccines (JnJ uses a human adenovirus,
whereas AZ/OX uses a simian adenovirus; the Russian Sputnik V vaccine uses two different
human adenoviruses). Perhaps the problem is related to viral vector
vaccines (called a “class effect”), since no such effect is seen for the mRNA vaccines
from Pfizer & Moderna? After all, there’s only 1 other viral vector vaccine approved
(JnJ’s Ebola vaccine, approved in Europe), so the data are thin on the ground.
Today, though, the US authorities announced similar, but very rare, effects from the JnJ
vaccine. Both JnJ and AZ/OX are viral vector vaccines (JnJ uses a human adenovirus,
whereas AZ/OX uses a simian adenovirus; the Russian Sputnik V vaccine uses two different
human adenoviruses). Perhaps the problem is related to viral vector
vaccines (called a “class effect”), since no such effect is seen for the mRNA vaccines
from Pfizer & Moderna? After all, there’s only 1 other viral vector vaccine approved
(JnJ’s Ebola vaccine, approved in Europe), so the data are thin on the ground.
It’s all over the popular media; I used reports from the venerable Globe [1] and the New York Times [2]. For somewhat higher technical accuracy and less of a miserable focus on “story”, we turn to the reliable Helen Branswell at STAT News [3] and the press release from the CDC’s director of CBER himself, Peter Marks [4].
Synthesizing the reports from these 4 articles, with of course more emphasis on the last 2, the situation is pretty clear:
- First, a weirdness: the FDA and CDC can say “hey, stop using this emergency medication while we figure out a safety problem”, but the states don’t have to listen! At the state level, boards of health can continue to do whatever they want with the vaccine they already have on hand. That’s… nuts. To my readers outside the US who may be thinking that health care in the US is crazy: why yes; yes, are correct in that conclusion.
- The precipitating event was noticing CSVT (like the AZ/OX thromboses in Europe) in 6
women, aged 18-48. There had been 6.8 million JnJ doses given at that point, so we’re
talking about a rare event (as in rarer than 1 in a million):
\(\begin{align*} d/dt \Pr(\mathrm{thrombosis.death} | \mathrm{vax}) & = (6/\mathrm{fortnight}) / 6.8 \times 10^{+6} \\ & = 8.82 \times 10^{-7}/\mathrm{fortnight} \end{align*}\) - The CDC Advisory Committee on Immunization Practice (ACIP) meets tomorrow. The FDA is investigating causes of the thromboses, oddly combined with low platelet counts (thrombocytopenia). The theory is that the vaccine might induce antibodies that activate platelets, leading to clots and low platelet counts.
- Signs to watch for in vaccinees: severe headache, shortness of breath, pain in legs/abdomen. All indicate a trip to the local ER.
- Heparin (an anti-coagulant)therapy is standard for thromboses, but inadvisable or even deadly here. Platelets are depleted and there may be PF4-heparin antibodies formed as the mechanism; non-heparin anti-coagulants are the order of the day. If so, might PF4-heparin antibodies be a tox biomarker to use for diagnosis?
- JnJ is about 5% of doses given in US so far. Pfizer & Moderna deliver 23 million doses/week without notable safety concerns (though with difficult cold chain requirements). The Biden administration is confident there will be enough vaccine in the US, even if we restrict it to Pfizer & Moderna (at 3 million doses/day, 23 million doses/week is just barely enough). Outside the US, particularly in the developing world where AZ/OX and JNJ are preferred because of handling issues, it’s an uglier story.
Some risk comparisons
Ok, so how serious is that risk of a probability rate of thromboses of $8.82 \times 10^{-7}$ per fortnight? Let’s compare with other risks to see if this is something to worry about, or do you have a greater chance of being run over by a car on your way to your vaccine appointment?
Some less silly comparisons:
-
Compare with COVID-19 death risk in US: In the first year of the pandemic, there were roughly 500k deaths in the US, in a population of about 328 million. Since we’re looking here at thromboses within 2 weeks of vaccination, we have to convert that to a probability per fortnight. Conclusion: There’s about 100x higher risk of COVID-19 death from not being vaccinated.
\(\begin{align*} d/dt \Pr(\mathrm{covid.death} | \mathrm{no.vax}) & = (500,000/\mathrm{yr}) / (328 \times 10^{+6} \cdot 26 \mathrm{fortnight}/\mathrm{yr}) \\ & = 5.86 \times 10^{-5}/\mathrm{fortnight} \end{align*}\) -
Compare with thrombosis risk in general in the US: The NYT article above cites the CDC saying there are 300k – 600k thrombosis cases per year in the US. Ok, so let’s convert that to a probability per person per fortnight for comparison. Conclusion: There’s about 100x higher risk of thrombosis in the general population.
\(\begin{align*} d/dt \Pr(\mathrm{thrombosis}) & = (300,000/\mathrm{yr} - 600,000/\mathrm{yr}) / (328 \times 10^{+6} \cdot 26 \mathrm{fortnight}/\mathrm{yr}) \\ & = 3.52 \times 10^{-5} - 7.04 \times 10^{-5}/\mathrm{fortnight} \end{align*}\)
- Compare specifically CSVT type thrombosis risk per year: Ok, so the risk of
thrombosis in general is higher, but what about specifically cerebral sinus vein
thromboses, which are rarer? Are we seeing too many of those? An article in Stroke
[5] places the risk (3-5x higher than previously believed)
at 15.7 per million per year. Convert that to risk per person per fortnight for
comparison. Conclusion: This is comparable to what’s being seen in the vaccinee population,
so it’s not obvious that we’re seeing abnormally many CSVT’s.
\(\begin{align*} d/dt \Pr(\mathrm{CSVT}) & = 15.7 \times 10^{-6}/\mathrm{yr} \cdot 1\mathrm{yr}/26 \mathrm{fortnights} \\ & = 6.04 \times 10^{-7}/\mathrm{fortnight} \end{align*}\)

- Compare with risk of blood clots from birth control pills: It’s well-known that birth
control pills carry a risk of blood clots for younger women, approximately the
population at risk here. An article on WebMD [6]
quantifies this risk for us at 0.3% to 1% for 10 years of exposure. Let’s convert that
to a risk per person per fortnight, to compare. Conclusion: Birth control pills
present 100x higher risk of blood clots than this vaccine.
\(\begin{align*} d/dt \Pr(\mathrm{clot} | \mathrm{birthcontrol}) & = (0.003 - 0.01)/10 \mathrm{year} \cdot 1 \mathrm{year}/26 \mathrm{fortnights} \\ & = 1.15 \times 10^{-5} - 3.85 \times 10^{-5}/\mathrm{fortnight} \end{align*}\)

-
Compare anaphylactic shock risk in Pfizer or Moderna vaccines: The mRNA vaccines appear to be quite safe, especially with no apparent thrombosis risk. There is, however, a slight risk of potentially lethal anaphylactic shock (basically an allergic reaction from Hell) within the first 15 minutes. Is that any worse than the CSVT risk of JnJ? The CDC’s Mortality and Morbidity Weekly Report (how’s that for a periodical title!) puts that risk at 21 cases in a sample of 1,893,360 first doses of Pfizer. [7] Conclusion: This is about 100x the risk of CSVT from JnJ.
\(\begin{align*} \Pr(\mathrm{anaphylaxis} | \mathrm{mRNA}) & = 21 / 1,893,360 \\ & = 1.1 \times 10^{-5} \end{align*}\) -
Compare with the thrombosis risk in the AZ/OX vaccine: The STAT News source [3] says in the UK, EU, and 3 other countries there have been 222 thromboses (moslty younger women) seen in 34 million vaccinees. Let’s assume that’s 222 observed in a fortnight of observation after vaccination, which is the only reasonable interpretation. Conclusion: This is about 10x the risk with JnJ.
\(\begin{align*} d/dt \Pr(\mathrm{thromb} | \mathrm{vax}) & = (222/\mathrm{fortnight}) / 34 \times 10^{+6} \\ & = 6.53 \times 10^{-6}/\mathrm{fortnight} \end{align*}\)
Conclusion… for now
It looks like the risks are in favor of using the JnJ vaccines. Comparing the rate of events in the 2 weeks post vaccination:
- You’re 100x more likely to die of COVID than of a JnJ associated CSVT.
- You’re 100x more likely to get a general thrombosis than anything associated with JnJ.
- You’re at about the same risk of CSVT whether you take the JnJ vaccine or not.
- You’re 100x more likely to get blood clots from birth control pills than JnJ.
- You’re 100x more likely to get anaphylactic shock from mRNA vaccines than CSVT from JnJ.
- You’re about 10x more likely to get CSVT from AZ/OX than from JnJ.
So overall, the risk of CSVT from the JnJ vaccine looks less than the risks of other reasonable behaviors, and no worse than the general risk of CSVT anyway.
However: Those are the risks to the general population; if the identification of younger women as a higher risk group for CSVT holds up (see ACIP meeting tomorrow!) then it makes sense to pause briefly and put in place 2 things:
- Direct patients experiencing severe headaches, difficulty breathing, or pain in legs or abdomen within 2 weeks of vaccination to go immediately to an ER; say what happened and mention the usual heparin therapy is not a good idea.
- Direct younger women away from JnJ and toward either Pfizer or Moderna.
The pause needs to be brief, because every day we force people to go unvaccinated, they’re exposed to risk of death or disability from COVID-19, and that risk is 100x the risk of CSVT from the JnJ vaccine.
We can’t tell if that’s exactly what’s happening now, but it does appear to be. Or so one may hope.
TBD: I really should add 95% confidence limits on the above probabilities, given how often I’ve whined at other people for not doing so! The 100x differences in probability are likely to be significant, but it’s always good to be explicit about that.
Addendum 2021-Apr-14
The formidable med-chem blogger, Derek Lowe, whose blog In the Pipeline is hosted at Science Translational Medicine, weighed in today with a short Q&A on the JnJ clot situation. [8] We seem to be pretty much on the same page.
The ACIP committee is meeting right now. I’m too burned out on COVID to liveblog it.
Addendum 2021-Apr-14 (evening)
The options the ACIP could choose amongst are:
- withdraw EUA for JnJ entirely
- impose population restrictions for JnJ (male, or female age > 50 yr)
- go back to full use of JnJ
The ACIP has voted to continue the “pause” for another 7-10 days, while more data is gathered. That’s… less than ideal, but it’s what’s there. I hope they’ll be able to look through more data, conclude option 2 is the way to go, and resume vaccinations. It won’t make a lot of difference in the US, but it will make a lot of difference elsewhere, where JnJ or AZ/OX or “nothing” are the available options.
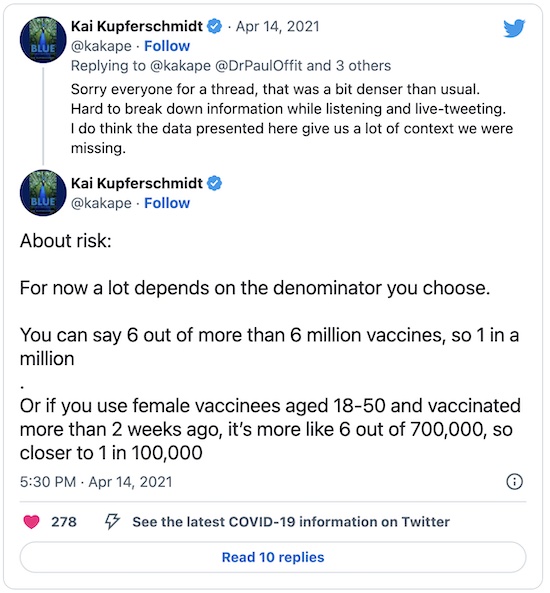
And as science journalist Kai Kupferschmidt points out, a lot of the risk assessments we did above depend on the denominator. Are we talking about population risk for all ~7 million JnJ vaccinees, or just the ~700k women age 18-50 vaccinated in the last 2 weeks? That changes the population by a factor of 10, and thus bumps up the thrombosis probability by 10x. The conclusion that the risk of CSVT is still less than the risk of COVID death is still approximately true, I think — but it makes the halt to examine subpopulations slightly more understandable.
Notes & References
1: Z Miller, “US recommends pausing Johnson & Johnson COVID-19 vaccine to investigate clotting reports”, Boston Globe, 2021-Apr-13. ↩
2: N Weiland, S LaFraniere, C Zimmer, “U.S. Calls for Pause on Johnson & Johnson Vaccine After Clotting Cases”, New York Times, 2021-Apr-13. ↩
3: H Branswell, “U.S. urges pause on use of Johnson & Johnson Covid-19 vaccine after rare blood clotting cases”, STAT News, 2021-Apr-13. ↩
4: P Marks (Director, CBER), “Joint CDC and FDA Statement on Johnson & Johnson COVID-19 Vaccine”, US FDA Press Announcements, 2021-Apr-13. ↩
5: S Devasagayam, et al., “Cerebral Venous Sinus Thrombosis Incidence Is Higher Than Previously Thought: A Retrospective Population-Based Study”, Stroke, 47 (2016-Jul-19), 2180-2182. DOI: 10.1161/STROKEAHA.116.013617.↩
6: N Todd, “Birth Control Methods and the Risk of Blood Clots”, WebMD, 2020-Mar-03. ↩
7: CDC COVID-19 Response Team, “Allergic Reactions Including Anaphylaxis After Receipt of the First Dose of Pfizer-BioNTech COVID-19 Vaccine — United States, December 14–23, 2020”, CDC Morbidity and Mortality Weekly Report, 2021-Jan-15. ↩
8: D Lowe, “Vaccine Side Effects Q and A”, In the Pipeline at Science Translational Medicine, 2021-Apr-14. ↩

Gestae Commentaria
Comments for this post are closed pending repair of the comment system, but the Email/Twitter/Mastodon icons at page-top always work.