COVID-19: Immunity Types and Real Prevalence
Tagged:COVID
/
JournalClub
/
Math
/
PharmaAndBiotech
/
SomebodyAskedMe
Two questions: what do we know about disease-induced vs vaccine-induced immunity, and what is the actual prevalence of COVID-19 beyond “officially reported” cases? Now there’s some data to think about here, though we can’t completely answer those questions.
Anti-nucleocapsid antibodies and vaccination
 Somebody asked me, indirectly via a friend,
about a recent medRχiv preprint on anti-nucleocapsid antiobodies in vaccinated
versus unvaccinated people. [1] A little
récherché, I thought, but it turned out the friend-of-a-friend’s real
question was far, far more bizarre than even my pessimistic imagination had suggested:
Somebody asked me, indirectly via a friend,
about a recent medRχiv preprint on anti-nucleocapsid antiobodies in vaccinated
versus unvaccinated people. [1] A little
récherché, I thought, but it turned out the friend-of-a-friend’s real
question was far, far more bizarre than even my pessimistic imagination had suggested:
… It’s not peer-reviewed yet, but there was a bombshell working paper released this month by the National Institute of Health, using Moderna’s own clinical trial data, that shows unvaccinated people develop significantly better immunity after Covid than people who have been vaccinated.
…
The study all-but-proves the mRNA shots themselves – and not whatever reduction in viral loads they may cause – are impeding the development of the anti-nucleocapsid antibodies.
…
According to the study, this could explain why vaccinated people get sick over and over, sometimes only months apart. The vaccine is a narrow defense for one specific virus mutation. Our natural antibodies are a broad defense. If the vaccine is messing with it, I think that’s ominous.
First impression: this looks like pure anti-vax madness from someone who doesn’t understand what an anti-nucleocapsid antibody is, when it is or is not relevant for immunity, and why it’s used in assays to measure community infection rates but not in vaccines. And who is willing to throw around wildly dangerous claims, very irresponsibly.
Still, let’s check out the paper to be sure.
The paper is in no way about the disease resistance of vaccinated versus unvaccinated people. Instead, it’s about measuring something called anti-nucleocapsid antibodies (antibodies to another part of the virus away from the spike protein) to get some idea of what fraction of the population has been exposed to the actual virus, not just the vaccine. That is, it’s about a public health assay.
Now it turns out that vaccinated people, when they have a breakthrough infection, generate less anti-nucleocapsid antibodies than the unvaccinated. So if you’re calibrating an assay to run on the population, there will be a lower positive-calling threshold in vaccinated people than in the vaccinated. The study is about getting this right.
There are lower anti-nucleocapsid antibodies in vaccinated people after breakthrough infection, because:
- Vaccinated people get sick less often (ample data to support this, so I can’t even imagine how an informed person would think otherwise),
- When they do get sick they have lower viral loads, clear the infection faster, and have less severe disease (again, ample data on hospitalization rates supports this), and
- Because they have such strong immune response via spike protein antibodies they more or less don’t bother forming anti-nucleocapsid antibodies.
Basically, for a vaccinated person there’s no point in making anti-nucleocapsid antibodies, because (a) the spike antibodies which they make in great quantity are usually enough to clear the infection, and (b) the nucleocapsid protein is inside the viral envelope where your immune system can’t see it until it’s infected a cell. So it’s pretty useless as a first-line defense.
The unvaccinated immune system just wildly makes antibodies to everything that looks viral, hoping something will work. The vaccinated immune system has been educated to attack the spike protein. So of course unvaccinated immune systems produce more of the relatively useless anti-nucleocapsid antibodies… to pretty much no effect.
Let’s examine some of the quantitative results from the paper:
- PCR-confirmed COVID-19 rates: Looking at all patients in either arm, how many got sick? 648/1298 = 49.9% of the placebo arm vs 21/491 = 4.3% of the vaccine arm. That is, vaccinated people ran about a 4% chance of infection vs 50% for unvaccinated over the same time period. Vaccinated people were 10x less likely to be infected! Vaccines are really, really good at suppressing sickness.
- Nucleocapsid ab levels: Looking at just the PCR-confirmed sickness cases, how many had nucleocapsid antibodies? 605/648 = 93% of the placebo arm vs 21/52 = 40% of the vaccinated arm. I checked using a statistical test called Fisher’s Exact Test, and yes this is statistically significant (not likely to be a fluke). However, all it means is that the immune systems of unvaccinated people struggled harder to clear the infection, making antibodies – even relatively useless ones like nucleocapsid antibodies. (Recall the nucleocapsid protein is inside the viral envelope, hence more or less useless to your immune system until the virus is actually inside a cell. The spike protein is outside the viral envelope, so your immune system can stop the virus before it gets in.)
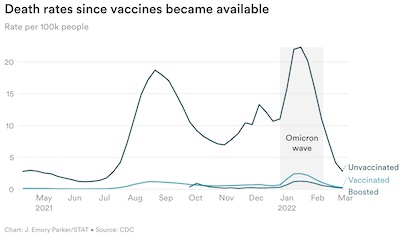 Vaccines do not lower your immunity. They are designed to do the opposite, and they do a
very good job of it. Consider the death rate in the US in the most recent wave,
stratified by vaccination status. The plot shown here, from STAT News, is the one we
used in a blog post on the day the US crossed 1 million official deaths.
It shows very clearly that very few of the deaths were among the vaccinated, and even
fewer among the boosted. This a stage of the pandemic in which the unvaccinated are
responsible for substantially all the deaths. Remaining unvaccinated is volunteering to
die, and attempting to bring down the rest of society with you.
Vaccines do not lower your immunity. They are designed to do the opposite, and they do a
very good job of it. Consider the death rate in the US in the most recent wave,
stratified by vaccination status. The plot shown here, from STAT News, is the one we
used in a blog post on the day the US crossed 1 million official deaths.
It shows very clearly that very few of the deaths were among the vaccinated, and even
fewer among the boosted. This a stage of the pandemic in which the unvaccinated are
responsible for substantially all the deaths. Remaining unvaccinated is volunteering to
die, and attempting to bring down the rest of society with you.
The bad news: Anti-vax crazies are wildly misinterpreting this paper, turning the calibration of a public health assay into some weird theory that unvaccinated people have better immunity. They do not.
The good news: The good guys are calibrating public health assays so we can get good, hard, reliable numbers on the rate of infection in the population in general. That’s hard now that everybody has at-home tests whose results they never report!
My friend’s informant is propagating dangerously nonsensical disinformation. I hope it’s through not understanding, rather than deliberate.
Limited cross-variant immunity from Omicron infection

 Still, that raises a question: is disease-induced immunity much good, even if it’s not as
good as vaccine-induced immunity?
Still, that raises a question: is disease-induced immunity much good, even if it’s not as
good as vaccine-induced immunity?
An article a couple weeks ago in Genetic Engineering & Biotechnology News [2] pointed to a paper in Nature [3] which addresses this.
The title is so good you (almost!) don’t need the rest: if you’re unvaccinated, you will get Omicron, and the Omicron-induced immunity has little effect on other variants. So you will get sick again.
Still, let’s listen to their words, not mine:
The question arises whether widespread Omicron infections could lead to future cross-variant protection, accelerating the end of the pandemic. Here we show that without vaccination, infection with Omicron induces a limited humoral immune response in mice and humans.
…
Sera from unvaccinated, Omicron-infected individuals show the same limited neutralization of only Omicron itself.
…
Our results demonstrate that Omicron infection enhances preexisting immunity elicited by vaccines but, on its own, may not confer broad protection against non-Omicron variants in unvaccinated individuals.
In other words: be safe, get vaccinated. And boosted.
A survey of COVID-19 incidence and paxlovid awareness
 Another question raised by the valiant attempt to make a nucleocapsid assay to measure
population infection rates: what is the real infection rate, anyway? Not just the
official, PCR-confirmed rate, because people test at home and the don’t report the
results.
Another question raised by the valiant attempt to make a nucleocapsid assay to measure
population infection rates: what is the real infection rate, anyway? Not just the
official, PCR-confirmed rate, because people test at home and the don’t report the
results.
Another medRχiv preprint landed last week, with a survey of New York City that attempts to answer this question. [4] Basically, they surveyed $N = 1030$ NYC residents of age over 18 years, by either smartphone or interactive land-line phone calls. I won’t go into the details, but they were careful to create a reasonably representative sample broken down by age, ethnicity, race, language spoken, borough of residence, and all the usual things.
There were a lot of survey questions, because it was carefully designed, but mostly it came down to verifying answers to a couple questions:
- Have you had COVID-19?
- Do you know about paxlovid therapy for COVID-19?
Some topline results:
- 22.1% (CL: 17.9% - 26.2%) had COVID in the last 2 weeks, about 1.5 million adults.
- 55.9% (CL: 44.9% - 67.0%) were unaware of paxlovid, so they could not ask for it.
- 15.1% (CL: 7.1% - 23.1%) received paxlovid, a small fraction of the obvious need.
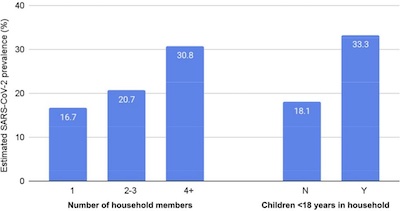 Interestingly, they call out 2 particular risk factors in Figure 1, shown here: living in
a larger group (e.g., family size), and the presence of children under 18 in the
household. More people probably means more chances to infect each other. Kids go
everywhere (not always masked), and can be asymptomatic carriers back to their families.
Interestingly, they call out 2 particular risk factors in Figure 1, shown here: living in
a larger group (e.g., family size), and the presence of children under 18 in the
household. More people probably means more chances to infect each other. Kids go
everywhere (not always masked), and can be asymptomatic carriers back to their families.
Also: higher infection in the Hispanic group and those less educated. Income, surprisingly, didn’t seem to matter much, nor did which borough of residence in NYC.
The Weekend Conclusion
- Anti-nucleocapsid antibodies are for a public health assay measuring population infection rates. They are meaningless about vaccination and disease resistance. You should still get vaccinated.
- Immunity from Omicron infection is pretty weak, and will not protect you from other variants much at all. You should still get vaccinated.
- A lot more people have COVID-19 than we think, and about half don’t know there is an effective therapy, which is being given out very reluctantly anyway. You don’t want to be in a situation where you need paxlovid, but are unable to get it. You should still get vaccinated.
Did I mention you should still get vaccinated?
Notes & References
1: D Follmann, et al., “Anti-nucleocapsid antibodies following SARS-CoV-2 infection in the blinded phase of the mRNA-1273 Covid-19 vaccine efficacy clinical trial”, medRχiv preprint, 2022-Apr-19. DOI: 10.1101/2022.04.18.22271936. ↩
2: GenEngNews Staff, “Omicron Infections, Without Vaccinations, Provide Little Immunity”, Genetic Engineering & Biotechnology News, 2022-May-19. ↩
3: RK Suryawanshi, et al., “Limited cross-variant immunity from SARS-CoV-2 Omicron without vaccination”, Nature, 2022-May-18. DOI: 10.1038/s41586-022-04865-0. ↩
4: SA Qasmieh, “The prevalence of SARS-CoV-2 infection and uptake of COVID-19 antiviral treatments during the BA.2/BA.2.12.1 surge, New York City, April-May 2022”, medRχiv preprint, 2022-May-26. DOI: 10.1101/2022.05.25.22275603. ↩

Gestae Commentaria
Comments for this post are closed pending repair of the comment system, but the Email/Twitter/Mastodon icons at page-top always work.