Ivermectin vs Strongyloidiasis Paper Published
Tagged:COVID
/
JournalClub
/
MathInTheNews
/
PharmaAndBiotech
/
SomebodyAskedMe
/
Statistics
Somebody asked me about the evidence associating putative ivermectin effects with worms, not COVID-19. Seems like it’s been finally published!
Remember those ivermectin meta-analyses?
Remember last fall when we looked at claims ivermectin worked against COVID-19, but the effect was pretty hinky when we looked at credible reviews? One of the main findings from Scott Alexander’s review [1] was from Avi Bitterman, showing the studies that showed an effect were in parts of the world with worm infestations:
Basically, worm infestations make everything more terrible, including COVID-19; removing the worms if present makes surviving COVID-19 more likely. But if you don’t have worms, then ivermectin does nothing for you.
Now it’s official!
Well, now Bitterman’s work has made it through peer review and is now officially in the
scentific literature. [2] Let’s have a quick look through
it:

- First, while there in theory a large number of studies available (199), only 12 made the final cut for inclusion, as we previously saw:
- 11 were duplicates,
- a whopping 175 were not proper randomized clinical trials (e.g., not randomized or no controls) or did not measure all-cause mortality as their primary outcome,
- 2 were excluded for outright fraud or randomization failure
- Statistically, the finding was pretty much that ivermectin looks like it might work if
your COVID-19 patients might have worms, but does not work in patients unlikely to
have worms. This is quantified by the Risk Ratio ($RR$), basically the ratio of rates of death
in ivermectin vs control arms. To achieve statistical significance, you’d like to see
$RR \le 1$ and the 95% confidence interval bounded below 1. This happenes
only in studies conducted in areas of the world with high worm infestations:
Ivermectin trials performed in areas of low regional strongyloidiasis prevalence18,19,29-32,35,37 were not associated with a statistically significant decreased risk of mortality (RR, 0.84 [95% CI, 0.60 - 1.18]; P=.31). By contrast, ivermectin trials that took place in areas of high regional strongyloidiasis prevalence17,33,34,36 were associated with a significant decreased risk of mortality (RR, 0.25 [95% CI, 0.09 - 0.70]; P=0.008).
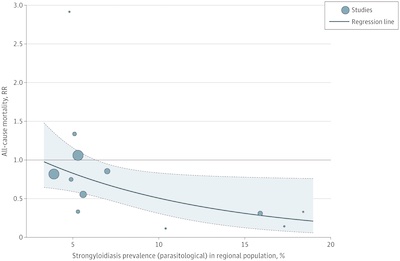
- Graphically, it looks like this: $RR$ is on the vertical axis, Strongyloides
infestation rate is on the horizontal axis, and each study is a dot (circle proportional
to study size).
- The curve is a regression model whose details I didn’t investigate (mixed-effects regression of $\log RR$ on Strongyloides infection rates). But note more importantly the confidence limits on $RR$: they’re only statistically significant in favor of ivermectin (i.e., below 1) in areas with more than about 8% of the population having worm infestations.
- The regression was statistically significance, and predicts a 38% drop in $RR$ for each 5% increase in worm prevalence.
The Weekend Conclusion
There’s more in the paper, but as far as I can tell the conclusion is that this finally, definitively closes the door on ivermectin as a COVID-19 therapeutic.
Ivermectin is for worms.
For COVID-19, seek first vaccination! Then, if you still get sick: seek paxlovid, molnupiravir, fluvoxamine, and monoclonal antibodies (one of the few remaining ones still effective against the Omicron variant, like bebtelovimab).
Notes & References
1: SA Siskind, “Ivermectin: Much More Than You Wanted To Know”, Astral Codex Ten Blog, 2021-Nov-07. ↩
2: A Bitterman, CP Martins, and A Cices, “Comparison of Trials Using Ivermectin for COVID-19 Between Regions With High and Low Prevalence of Strongyloidiasis: A Meta-analysis”, JAMA Netw Open 5:3, 2022-Mar-21, e223079. DOI: 10.1001/jamanetworkopen.2022.3079 ↩

Gestae Commentaria
Comments for this post are closed pending repair of the comment system, but the Email/Twitter/Mastodon icons at page-top always work.